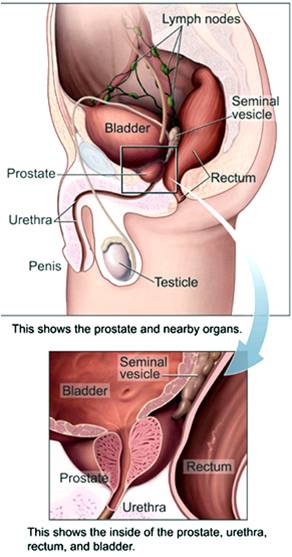
The prostate gland plays a pivotal role in men's health, and its well-being is often a topic of great concern, especially when it comes to prostate cancer, a leading cause of death among men in the United States. This article delves into the intricacies of prostate health, detection methods for prostate cancer, and the debated connection between testosterone replacement therapy (TRT) and prostate cancer.
Prostate Cancer Prevalence and Detection
As men age, the occurrence of small, hidden prostatic lesions increases, which could potentially turn cancerous over time. The prevalence of these lesions is around 30% in American men aged over 45, and this figure soars to over 80% for those above 80 years of age. The transformation of these lesions into cancerous cells is often linked to genetic factors and lifestyle conditions, including diet.
To detect prostate cancer, healthcare providers employ a variety of methods:
- Prostate-Specific Antigen (PSA) assays (for accurate test results, no ejaculation during the 24 hours preceding the test)
- Digital Rectal Examination (DRE)
- Transrectal Ultrasound
It's advisable for men, especially those above 40 or with a family history of prostate cancer, to undergo a DRE before commencing testosterone replacement therapy and every six months thereafter. While DRE may be uncomfortable, it's a small price to pay for ensuring good health. Any abnormal rectal exam findings, a PSA increase of more than 2 ng/mL, or a PSA level over 4 ng/mL usually necessitate further evaluation by a urologist, often involving an ultrasound and prostate biopsies.
However, the PSA and DRE methods lack sensitivity and specificity. In some instances, benign prostatic hyperplasia (BPH), a non-cancerous inflammation, may falsely elevate PSA levels, while 25% of prostate cancer patients show normal PSA levels. As it turns out, needle biopsies can find hidden prostatic lesions in men whose PSA levels and ultrasound results are normal.
Testosterone Replacement Therapy and Prostate Cancer: Unveiling the Connection
The role of Testosterone Replacement Therapy (TRT) in PSA elevation or prostate cancer development has been a topic of considerable debate. Prostate cancer is initially androgen-dependent; thus, TRT is discouraged for men diagnosed with prostate cancer. However, a comprehensive analysis encompassing data from 18 studies revealed no significant link between blood levels of androgens and an increased risk for prostate cancer (Journal of the National Cancer Institute, 2008). Intriguingly, some emerging data suggest that high doses of testosterone may be beneficial in treating certain types of prostate cancer.
A different study that looked at 149,354 men who were diagnosed with prostate cancer between 1991 and 2007 found that those who were treated with TRT did not have higher rates of death or use of Androgen Deprivation Therapy (ADT). The study, published in the Journal of Sexual Medicine (2014), concluded that TRT, post-prostate cancer diagnosis and treatment, doesn't exacerbate mortality rates or the necessity for ADT, even with prolonged TRT duration.
Conclusion
The dialogue surrounding prostate cancer, its detection, and the implicated role of TRT is complex. While the journey towards unambiguous understanding continues, regular screenings and open discussions with healthcare providers remain crucial for maintaining prostate health and making informed treatment decisions.
For more insights on this topic, refer to: Does Testosterone Cause Prostate Cancer? Can Men Treated for Prostate Cancer Use TRT?